CONCLUSION
|
This study investigated the role of metformin in the gluconeogenesis pathway, specifically observing its interaction with PC in the initial steps of mitochondrial gluconeogenesis. Metformin was found to inhibit PC, although not under the pharmacokinetic concentrations of 250µM-500µM. Additionally, 13C-NMR analysis indicated an interaction between metformin and biotin, the prosthetic group of PC, such that a carbonyl group was lost. The proposed metformin-biotin interaction is a transamination reaction, in which one of biotin’s carbonyl groups, specifically the one which binds to PC and activates it, is lost and is replaced with an amine group. Although an amine group was not found in the 13C-NMR of metformin mixed with biotin, the loss of one carbonyl in this interaction suggests support for the PC inhibition theory. If metformin somehow interacts with biotin, it is possible that this interaction prevents biotin from interacting with PC in mitochondrial gluconeogenesis, thereby preventing PC from completing its function in the pathway, leading to gluconeogenic inhibition.
|
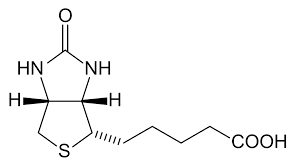
Figure __: Chemical structure of biotin.
|
|
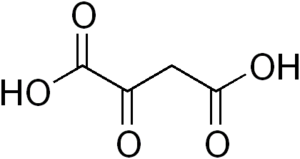
Figure __: Chemical structure of pyruvate carboxylase.
|
Further study should investigate the role of concentrations in metformin action, as several studies which support various mechanisms of metformin action find significance in a wide range of concentrations — some of which are suprapharmacokinetic, or outside the pharmacokinetically realistic range of concentrations. Furthermore, replication studies using a greater number of assay trials should be conducted in order to gain a more complete picture of metformin action in mitochondrial gluconeogenesis. Furthermore, in vitro or in vivo studies with metformin should be conducted in order to better model biological conditions, as these conditions may affect metformin action. Various other proposed targets of metformin action, such as AMPK or GPDH, should be investigated, and these findings should be compared to those of the present study. Various other uses of metformin, such as cancer treatment, should be investigated in order to amass more knowledge on the drug profile and various mechanisms of action in the body. Furthermore, a comparative study between metformin and other biguanides, as well as between biguanides and other antidiabetic drug groups, should be conducted in order to amass more knowledge for the field and help to engender more options for the treatment of type II diabetes as well as other diseases.
|
|
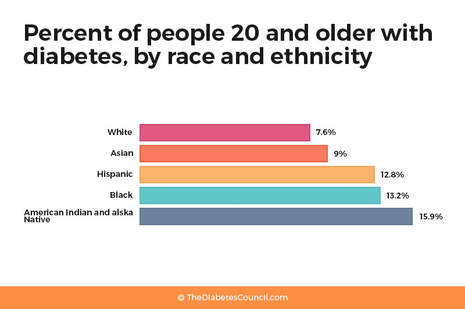
These study findings pose important implications for the field of public health. Type II diabetes is a disease which may be caused and worsened by several socioeconomic factors, such as food insecurity, which is the inability to afford or access nutritious foods. This can lead to a diet high in sugars, which can cause obesity and prediabetes, two powerful precursors for the development of type II diabetes. Metformin is a first line drug of choice due to its relative safety and accessibility, and is the most commonly prescribed drug for the treatment of type II diabetes. A common side effect of metformin known as lactic acidosis can lead to severe, debilitating pain and cramping (Duong et al., 2013). Given that type II diabetes disproportionately affects Native Americans, African Americans, and Latinos/Hispanics - the three ethnic demographic groups which face the lowest socioeconomic status (SES) in the United States (Macartney, Bishaw & Fontenot, 2013; Spanakis & Golden, 2014) - lactic acidosis is particularly harmful, as it prevents working people in lower socioeconomic levels from being able to work and earn a livelihood necessary for obtaining basic health care and other such amenities. Understanding the mechanism of metformin action will not only add to the growing body of knowledge in the field, but will allow for more and better treatment options to be uncovered, as well as will help to explain and ameliorate symptoms such as lactic acidosis.
|